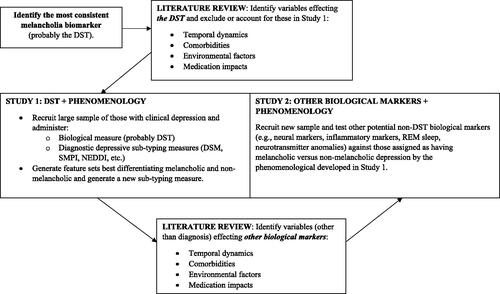
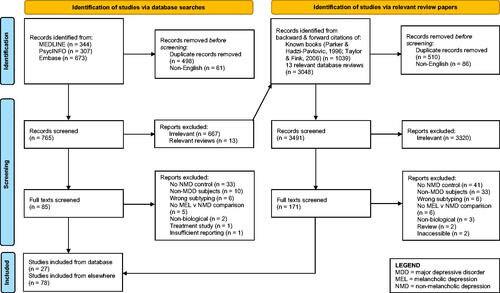
Figures & data
Table 1. Search strategy for MEDLINE, PsycINFO, and EMBASE.
Table 2. Definitional criteria for melancholia.
Table 3. Summaries of studies exploring endocrinological markers of melancholia.
Table 4. Summaries of studies concerning neurological biomarkers of melancholia.
Table 5. Summaries of studies exploring immunological markers of melancholia.
Table 6. Summaries of studies exploring metabolic markers of melancholia.